Every May, the phone at the clinic begins to ring a little differently.
People tell us they look tired, their under-eyes have changed, and that friends have asked if they have been sleeping well. They’ve often been sleeping perfectly well. What’s changed is the pollen count.
According to the Met Office pollen forecast, UK grass pollen peaks from mid-May through July, with the heaviest concentrations usually in early June. For many people, that means weeks of low-grade facial inflammation that doesn’t always announce itself as hay fever (allergic rhinitis).
There might not be a runny nose, nor any obvious sneezing fits. Just a face that doesn’t quite look like itself in the mirror.
This guide is for the patients we see in spring who suspect ageing and are actually dealing with an allergy. The distinction matters because the answer to one is patience and appropriate medical care, and the answer to the other is something else entirely.
What Hay Fever Face Actually Is
When pollen enters the airways and the tissue around the eyes, the immune system recognises it as a threat. Mast cells in the lining of the nose, sinuses and conjunctiva (the membrane covering the white of the eye) release histamine. Histamine then does what it is supposed to do: it makes nearby blood vessels widen and become more permeable, so that immune cells can flood into the area and deal with the perceived invader.
The problem is the location. The skin around the eyes is the thinnest on the body, approximately 0.5 millimetres. The tissue underneath it is loose and well supplied with small vessels.
When those vessels dilate and leak fluid, the surrounding area swells quickly and clearly. The pooling of blood in the dilated vessels also shows through that paper-thin skin as a bluish or violet shadow. This shadow is known as an allergic shiner, or a dark circle.
The package usually includes puffy upper or lower lids, watery red eyes, a faint flush across the cheeks and nose, and sometimes a slightly swollen, heavier look to the entire face. None of it is structural. All of it is reversible.
How to Tell Hay Fever Face From Ageing
- Symptoms began within days of high pollen days, not over months
- Symptoms are worse first thing in the morning and after time spent outdoors
- Both sides of the face are affected equally
- Sneezing, throat irritation or nasal congestion accompany the facial changes
- A non-drowsy antihistamine reduces the swelling within a day or two
Why We See a Spike in Tired Eye Enquiries Every May
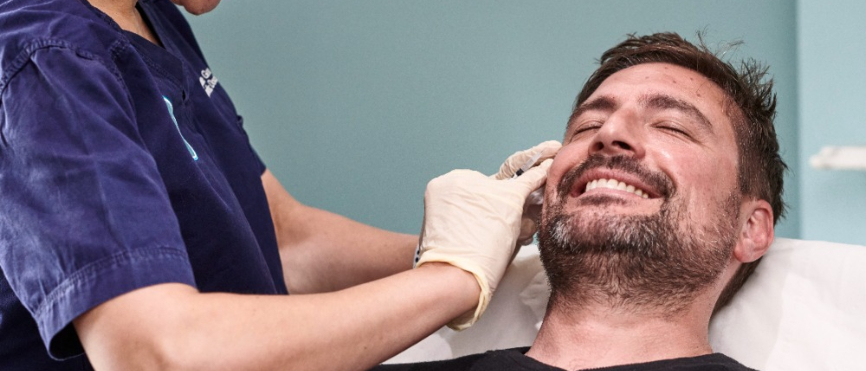
At the clinic, we see a pattern from late April onwards. Patients book consultations for tear trough filler, under-eye polynucleotides or anti-wrinkle treatment around the eyes, often with a phone photo showing how tired they look. In a lot of these consultations, the underlying issue isn’t volume loss. It’s an allergic swelling, and treating the wrong problem will not fix it.
A consultation that takes this seriously will pause before booking anything. We routinely decline to treat under-eye concerns during an active allergic flare, and we will say so on the day. It saves people from spending money on a treatment that can’t answer the question they are actually asking.
What Not to Do During an Active Flare
Injectable treatments around the eyes should be postponed. There are three reasons:
- The vessels dilate and become more prone to bruising
- The tissue is swollen, which distorts the assessment of where the volume actually sits
- Any result placed into the inflamed tissue will not reflect the face you have once the inflammation settles
Avoid using aggressive skincare, such as retinoids, glycolic and salicylic acids, and strong vitamin C serums, as they can aggravate an already-irritated skin barrier. This is a season for ceramides, panthenol and hyaluronic acid, not for pushing the skin harder.
And, gently but firmly: try not to rub the eyes. Mechanical friction triggers further histamine release, which exacerbates the swelling, and it damages the delicate skin in a way that genuinely does, over the years, contribute to fine lines and pigmentation.

What Genuinely Helps in the Short Term
Most patients can manage hay fever face well at home with a combination of the following. None of this is a clinic treatment. All of it is supported by NHS and Allergy UK guidance.
A cold compress applied for several minutes constricts the dilated vessels and reduces the fluid leak. A clean flannel rinsed in cold water, or a gel mask kept in the fridge, works well. Avoid anything frozen directly against the skin.
A non-drowsy antihistamine such as cetirizine, loratadine or fexofenadine, taken consistently through the season, is more effective than reaching for one only when symptoms appear. Continuous low-level blockade keeps the histamine cascade quieter. A pharmacist can advise on which formulation suits you.
A saline rinse or saline nasal spray clears pollen from the nasal lining, which lowers the total allergen load reaching the upper airway. Eye drops containing sodium cromoglicate or ketotifen are useful when eye symptoms are the main complaint and can be bought over the counter.
Wraparound sunglasses are quietly one of the most effective interventions outdoors, simply by reducing the amount of pollen that reaches the conjunctiva. Washing the face and changing the pillowcase after time outside means you are not sleeping with pollen pressed against your skin for eight hours.
For skincare, keep it short and supportive. A gentle cleanser, a barrier-supporting moisturiser with ceramides or panthenol, and a hyaluronic acid serum for hydration are enough. SPF in the morning, always.
When to See a GP
Self-care is sufficient for most people, but there are situations where a GP visit is the right next step. Severe or persistent symptoms that disrupt sleep, hay fever combined with asthma or worsening asthma control, or symptoms that do not respond to over-the-counter antihistamines all warrant a conversation with a doctor.
GPs can prescribe stronger antihistamines, combination nasal sprays containing a steroid and an antihistamine, or short courses of oral steroids in severe cases. For patients with significant, recurrent symptoms that affect quality of life, referral for immunotherapy may be appropriate. The NICE Clinical Knowledge Summaries on allergic rhinitis are a standard reference your GP will be working from.
What a Doctor Would Consider Once the Flare Has Settled
Once the pollen season ends or symptoms are well controlled on a stable antihistamine regimen, it becomes possible to assess the face properly. We usually wait until symptoms have been settled for a sustained period before evaluating any under-eye concerns. From there, a conversation about options would take place.
Lymphatic drainage, for example, with Body Ballancer compression therapy, can help shift residual periorbital congestion in patients who feel puffiness stays around after the flare.
Polynucleotides under the eye are considered to improve the quality of skin that has been repeatedly stretched and inflamed over many seasons.
Tear trough filler is indicated only where there is genuine volume loss above the cheek, separate from any allergic fullness, and a careful assessment can distinguish the two.
Anti-wrinkle injections have a particular relevance here. Years of squinting against pollen, rubbing irritated eyes, and frowning through congestion laid down expression lines around the eyes and between the brows. These respond well to treatment once active inflammation has resolved.
LED phototherapy, such as Dermalux, can help with residual redness and support barrier recovery in the weeks after a heavy season.
All of these are options to discuss in a consultation with us.
Frequently Asked Questions
Does hay fever cause permanent dark circles?
The shadowing from allergic shiners is not permanent in itself. However, rubbing the eyes and stretching the thin periorbital skin over time might result in long-term pigmentation and skin thinning. Treating the allergy well each season is the best prevention.
Can I have Botox during hay fever season?
We would generally advise waiting until an active flare has settled. Injecting into inflamed, swollen tissue increases bruising risk and makes accurate assessment harder. If you are well controlled on antihistamines and have no active symptoms on the day, treatment elsewhere on the face is usually fine; the eye area specifically is where we pause.
Why is my face puffier on one side?
Allergic swelling is often symmetrical, but the side you sleep on can be more affected in the morning because of how fluid pools overnight. Persistent one-sided swelling that does not match the other side as the day progresses is worth mentioning to a GP, as it can occasionally indicate something other than an allergy.
Does hay fever make my skin age faster?
Repeated rubbing of the eye area, chronic mild inflammation, and disturbed sleep from severe symptoms can all contribute to the appearance of premature ageing around the eyes. Controlling the allergy well, protecting the skin barrier, and avoiding rubbing are meaningful interventions.
How long after a flare should I wait before having tear trough filler?
There’s no fixed waiting period, but the under-eye area needs to be back to its baseline before we assess or treat it. Injecting into swollen tissue distorts what we’re correcting and means the result won’t reflect your actual anatomy. In practice, that usually means waiting until symptoms are well-controlled and any puffiness has fully settled. This is often a couple of weeks after a significant flare.
A Final Note
Hay fever face is temporary. The swelling settles, the shadows fade, and the face you recognise comes back. If symptoms persist beyond the pollen season, or you suspect there is a structural component sitting underneath the allergy, a consultation is the right place to begin. We will give you an honest assessment of what an allergy is and what its anatomy is, and we will not suggest a treatment you do not need.